The H5N1 bird flu virus has infected more than 70 people in the United States since 2024, killed millions of commercial poultry birds, and spread through nearly a thousand dairy herds across 17 states. If you're wondering whether you should be worried, here's the honest answer: the CDC says the general public risk is low, but the virus is now widespread enough in animals that knowing how to protect yourself actually matters.
You don't need to panic. You do need to know a few specific things about how this virus spreads, who's actually at risk, and what practical steps keep you safe. This guide covers exactly that, based on the most current CDC data as of February 2026.
Where H5N1 Stands Right Now
The numbers tell a clear story about where this virus lives and who it affects. As of February 18, 2026, the CDC has confirmed 71 human cases of A(H5) bird flu in the United States. Of those, 41 cases came from exposure to infected dairy cows, 26 from infected poultry, and the rest were detected through routine flu surveillance. Two people have died, including a Louisiana resident over 65 with underlying health conditions who had contact with backyard poultry.
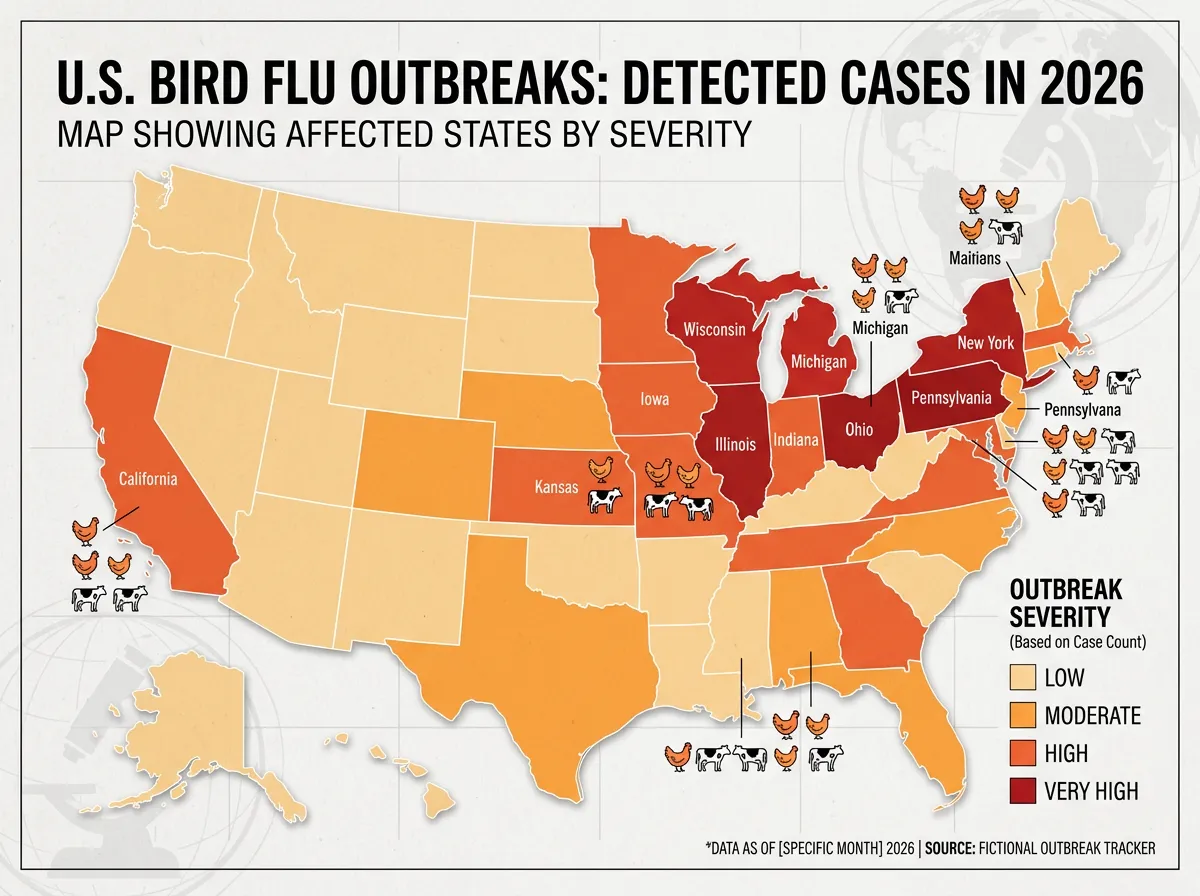
The animal side of the outbreak is far larger. Bird flu has been detected in 28 states since the beginning of 2026, with over 4.8 million birds affected in January and early February alone. A single Colorado facility lost 1.3 million birds, and a Pennsylvania farm lost 1.5 million hens. Since March 2024, 989 dairy herds in 17 states have confirmed infections. Maurice Pitesky, a poultry disease expert at UC Davis, put it bluntly: "It's global and ubiquitous at this point, and by every definition that I know of, it's endemic."
The important distinction is this: no confirmed person-to-person transmission has occurred with the H5N1 strains currently circulating in the US. Every human case has been traced back to direct animal contact. That's why the CDC keeps the public risk assessment at "low," while simultaneously monitoring the situation closely and urging people who work with animals to take precautions seriously.
Who Actually Needs to Worry
The risk isn't evenly distributed. If you don't have regular contact with poultry, wild birds, or dairy cattle, your personal risk is extremely low. But certain groups need to take active precautions.
Dairy farm workers face the highest documented risk. They account for 41 of the 71 confirmed US cases because milking infected cows involves close, prolonged contact with animals shedding the virus. Many of these workers face additional barriers to getting tested and treated, including documentation concerns, language barriers, and lack of paid sick leave. Poultry farm workers represent the second-largest group at 26 cases, particularly those involved in depopulation efforts at infected facilities.
Backyard flock owners are a less obvious but real risk group. The first US death from this outbreak involved someone who kept backyard chickens. Unlike commercial operations, backyard setups rarely have biosecurity protocols, and owners handle their birds directly and frequently. Hunters who handle wild waterfowl, veterinarians working with potentially infected animals, and anyone involved in wildlife rehabilitation also face elevated exposure.
For everyone else, the primary risk comes not from breathing the same air as a sick bird but from specific behaviors: touching dead wildlife, handling raw poultry carelessly, or drinking unpasteurized milk from potentially infected herds.
Step-by-Step Protection for Everyday Life
The CDC's prevention guidance boils down to a set of practical habits that don't require any special equipment or lifestyle changes for most people. Here's what to do, organized by where you're most likely to encounter risk.
In your kitchen, cook all poultry to an internal temperature of 165°F (74°C), which kills H5N1 and every other foodborne pathogen you'd encounter. Cook eggs until both the white and yolk are firm. Choose pasteurized milk and dairy products. The USDA and FDA have confirmed that pasteurization eliminates the virus, so commercially sold milk is safe. If you buy from a local farm, ask whether they pasteurize. If they don't, and their herd hasn't been tested, consider switching sources during active outbreaks in your state.
Outdoors, avoid touching wild birds, whether alive or dead. This applies to songbirds at your feeder, waterfowl at parks, and any bird you find on the ground. If you need to dispose of a dead bird on your property, the CDC recommends using gloves or turning a plastic bag inside out over your hand, picking up the bird, sealing it in a garbage bag, and placing it in your regular trash. Wash your hands thoroughly with soap and water afterward.
Around animals, keep your distance from visibly sick livestock. If you visit farms, petting zoos, or agricultural fairs, wash your hands immediately after any animal contact. Don't touch surfaces that may be contaminated with animal droppings, feathers, or bedding.

What Backyard Flock Owners Should Do Now
If you keep chickens, ducks, or other poultry at home, your risk profile is different from the general public, and the steps you need to take are more specific. Start by limiting contact between your birds and wild waterfowl, which are the primary carriers. Cover outdoor runs with netting to prevent wild birds from entering. Store feed in sealed containers that wild birds and rodents can't access. If you notice any of your birds acting lethargic, producing fewer eggs, developing swollen heads, or dying unexpectedly, don't handle them without protection.
The minimum protective equipment for handling potentially sick birds includes disposable gloves, eye protection (goggles or a face shield, not just glasses), and an N95 respirator or equivalent. Wear dedicated shoes or boot covers that stay in the coop area. Change clothes before entering your home. These sound like overkill until you remember that the first American to die from H5N1 in this outbreak was a backyard flock owner.
Report any unusual deaths in your flock to your state veterinarian or call the USDA at 1-866-536-7593. Early detection matters for containing spread to neighboring flocks and for your own health. If you develop flu-like symptoms (fever, cough, body aches, eye redness) within 10 days of contact with sick or dead birds, contact your healthcare provider immediately and mention the exposure. Antiviral treatment with oseltamivir (Tamiflu) is most effective when started within 48 hours of symptom onset.
The Vaccine Question
There is no H5N1 vaccine available to the general public in the United States right now. The federal government has stockpiled H5N1 vaccines that show 60-95% seroconversion rates against the current clade 2.3.4.4b virus, and planning is underway for a potential public vaccination campaign if the situation changes. But "if" is doing heavy lifting in that sentence.
On the research front, scientists at Washington University School of Medicine in St. Louis have developed a nasal spray vaccine that blocks bird flu infection in animal testing. Dr. Michael S. Diamond, one of the lead researchers, explained that "delivering vaccine directly to the upper airway where you most need protection from respiratory infection could disrupt the cycle of infection and transmission." The nasal approach is promising because it could prevent infection at the entry point rather than just reducing severity, but it's still in early research stages with no timeline for human trials.
For poultry, Zoetis has received conditional approval for a bird vaccine targeting H5 influenza. At least seven vaccine candidates for cattle are approved for field safety trials. These animal vaccines matter because reducing the virus in livestock reduces the chances of human exposure, which is the real-world path to controlling this outbreak.
In the meantime, the CDC recommends getting your regular seasonal flu vaccine. It won't protect against H5N1, but it reduces your risk of co-infection with both seasonal flu and bird flu simultaneously, which could be more dangerous and would complicate diagnosis.

Why Experts Say We're Not Ready
The low public risk assessment comes with a significant caveat: the infrastructure needed to respond if H5N1 mutates to spread between humans is weaker than it should be. Brian Castrucci, an epidemiologist and president of the de Beaumont Foundation, has been direct about the gap: "The U.S. is underprepared for bird flu because we have not learned our lessons from COVID." His organization's analysis found that the country needs at least 80,000 more public health staff to deliver basic services, let alone mount a rapid response to a new pandemic threat.
Jessica Malaty Rivera, an epidemiologist and science communications adviser at the same foundation, has raised concerns about surveillance gaps: "Evidence suggests the outbreaks first emerged late last year, which means we're likely not seeing the full scale of the situation." The worry isn't that H5N1 is currently a crisis for the average person. The worry is that every undetected animal infection is another opportunity for the virus to mutate, and the systems designed to catch that mutation early are stretched thin.
This context matters for your personal decisions. The practical steps in this guide protect you today. But they also mean you won't become an undetected link in a chain of transmission if the virus does change, which is the quiet public health benefit of individual precaution.
What to Remember
The bird flu situation in 2026 calls for awareness, not alarm. The virus has not developed the ability to spread between people, and every human case traces back to direct contact with infected animals. Your risk as a member of the general public remains low.
The protective steps are straightforward: cook poultry and eggs thoroughly, choose pasteurized dairy, avoid touching wild or sick birds, and wash your hands after any animal contact. If you keep backyard poultry, treat biosecurity as non-negotiable and report any unusual bird deaths. If you work with livestock, use proper protective equipment every time, not just when you think an animal looks sick.
There's no available public vaccine yet, but seasonal flu shots still matter, and research on H5N1-specific vaccines is advancing. The best thing you can do right now is stay informed through the CDC's bird flu situation page, which updates regularly as the outbreak evolves.
Sources
- A(H5) Bird Flu: Current Situation Summary - CDC, updated February 18, 2026
- Preventing Bird Flu Infections in People - CDC
- Bird Flu Cases Are Surging in 2026 - Sentient Media, February 2026
- New Nasal Vaccine Shows Strong Protection Against H5N1 Bird Flu - ScienceDaily, February 4, 2026
- US "Underprepared" for Bird Flu Outbreak, Epidemiologists Warn - Newsweek

