With Lent starting today and millions of people beginning a 40-day fast of some form, the perennial question is back: does fasting actually help you lose weight? The internet is full of confident answers in both directions, from enthusiastic proponents who credit intermittent fasting with transforming their health to skeptics who call it a rebranded version of skipping meals. The research, as it often does, tells a more complicated story.
The verdict: partially true, with significant caveats. Fasting can lead to weight loss, but the latest evidence suggests it works primarily because it reduces total calorie intake, not because of any metabolic magic specific to when you eat. A major Harvard analysis published in June 2025, covering 99 clinical trials and more than 6,500 participants, found that intermittent fasting and traditional calorie-restricted diets produced comparable weight loss results. A separate Cochrane review published in February 2026, analyzing 22 randomized clinical trials, concluded that intermittent fasting showed no clinically meaningful advantage over standard dietary advice. The weight comes off, but the mechanism is calories in versus calories out, not the fasting window itself.
What "Intermittent Fasting" Actually Means
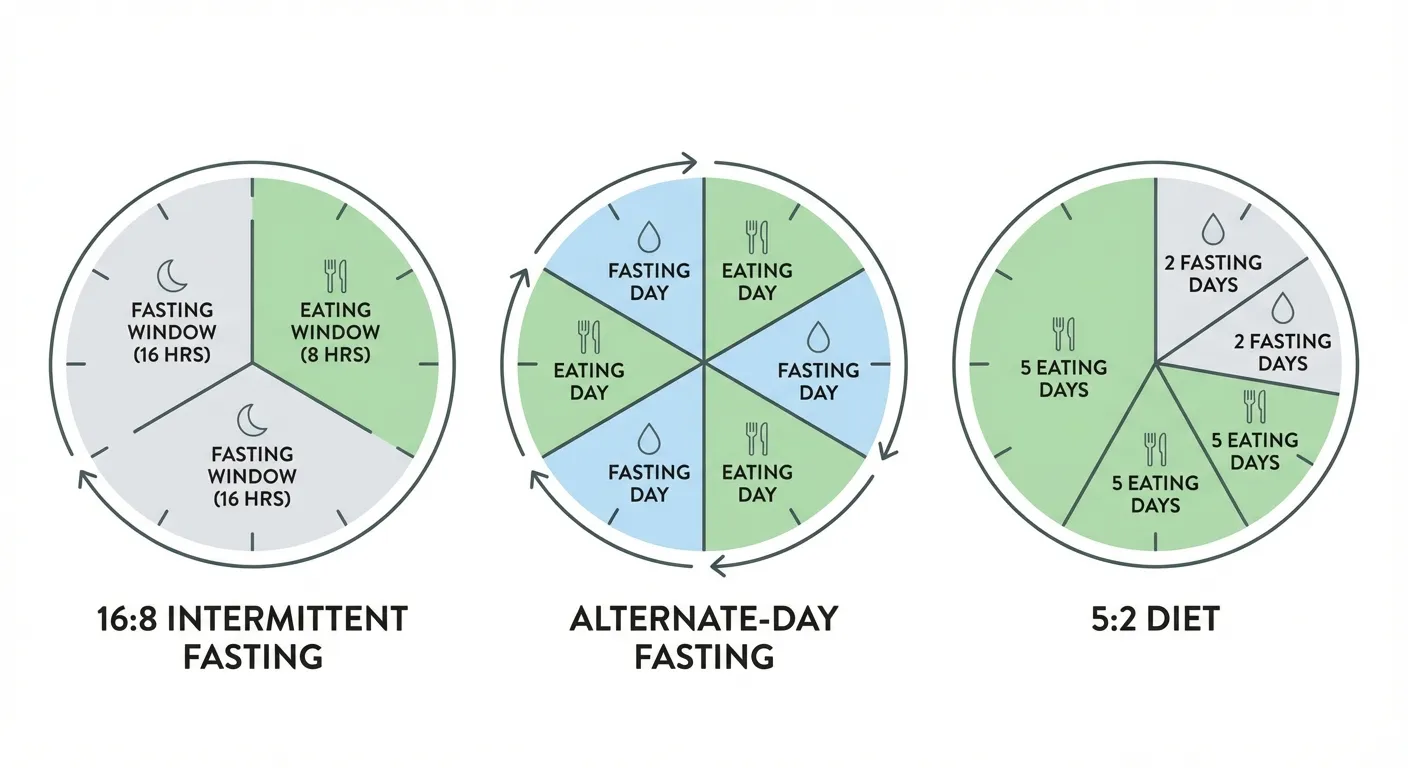
The term covers several distinct approaches, and lumping them together is one of the biggest sources of confusion in the research. The three most common protocols are time-restricted eating, alternate-day fasting, and the 5:2 method, and they produce different results in different populations.
Time-restricted eating (TRE) is the most popular version. You eat all your meals within a set window, typically 8 hours (the "16:8" pattern), and fast for the remaining 16 hours. A stricter version narrows the eating window to 6 or even 4 hours. The appeal is simplicity: no calorie counting, no food restrictions, just a clock. Most people who say they're doing "intermittent fasting" mean some form of time-restricted eating.
Alternate-day fasting (ADF) involves eating normally one day and either fasting completely or eating very little (around 500 calories) the next. This approach has the strongest research base for weight loss, partly because the calorie reduction is substantial by design. It's also the hardest to sustain long-term, which limits its practical usefulness.
The 5:2 method allows normal eating five days per week and restricts intake to 500-600 calories on two non-consecutive days. It's a compromise between daily restriction and alternate-day fasting, and adherence rates tend to be higher than ADF in studies lasting more than three months.
Understanding these distinctions matters because a study showing that "fasting works" using alternate-day fasting doesn't necessarily mean that skipping breakfast (a loose form of time-restricted eating) will produce the same results. Much of the popular confusion about fasting's effectiveness comes from extrapolating findings across protocols that differ dramatically in actual calorie reduction. If you're exploring fasting as part of a Lenten observance that starts today, the religious practice is quite different from any of these clinical protocols.
What the Strongest Studies Actually Found
The most authoritative evidence on fasting and weight loss comes from three recent analyses that together paint a clearer picture than any single study.
The Harvard T.H. Chan School of Public Health published a comprehensive umbrella review in June 2025, synthesizing data from 99 randomized controlled trials involving 6,532 adults with overweight or obesity. The review found that intermittent fasting significantly reduced body weight by an average of 3.73 kilograms (about 8.2 pounds) and lowered BMI compared to unrestricted diets. However, when compared directly to continuous calorie restriction (traditional dieting), the results were statistically equivalent. In other words, fasting worked, but it didn't work better than simply eating less every day.
The ChronoFast study, published in January 2026 in ScienceDaily's research coverage, tested a specific hypothesis: does time-restricted eating provide metabolic benefits beyond calorie reduction? Researchers had participants follow a time-restricted eating pattern without reducing their total calorie intake. The result was striking: no clinically meaningful changes in insulin sensitivity, blood sugar, blood lipids, or inflammatory markers. "The health benefits observed in earlier time-restricted eating studies were likely attributable to unintended calorie reduction rather than the shortened eating window itself," the researchers concluded. This is a critical finding because it undercuts the popular claim that fasting triggers unique metabolic pathways that enhance weight loss independently of calorie deficit.
The Cochrane review published in February 2026 added another layer. Analyzing 22 randomized clinical trials, it concluded that intermittent fasting "did not appear to have a clinically meaningful effect on weight loss compared to standard dietary advice." As Euronews Health reported, the review's lead authors noted that while some participants did lose weight on fasting protocols, the magnitude was not significantly different from what conventional dietary guidance achieved.
The consistent takeaway across all three analyses is the same: fasting is a valid method for creating a calorie deficit, but the fasting itself isn't the mechanism. The calorie deficit is. This doesn't mean fasting is useless. For people who find it easier to restrict when they eat rather than what they eat, it's a legitimate tool. But the metabolic claims that permeate fasting culture online, that restricting your eating window "resets" your metabolism, "unlocks" fat burning, or "activates autophagy" in ways that simple calorie restriction doesn't, are either unproven or have been directly contradicted by recent evidence.
The Muscle Loss Problem
One of the most persistent concerns about fasting is muscle loss, and the research here is genuinely worth paying attention to. A 2021 analysis published in Frontiers in Nutrition described intermittent fasting as "a suboptimal dietary strategy for supporting muscle protein remodeling and muscle mass," particularly in populations already at risk for muscle loss.
The core issue is protein timing and distribution. Muscle protein synthesis is stimulated by consuming dietary amino acids, and research suggests that spreading protein intake across three to four meals separated by three to five hours optimizes this process. Compressing all eating into a 6- to 8-hour window makes it difficult to space protein intake effectively, particularly for people trying to consume the recommended 1.6 grams of protein per kilogram of body weight daily.
That said, the picture isn't entirely bleak. A 2024 study in Clinical Nutrition found that short-term intermittent fasting with adequate total protein intake did not impair muscle protein synthesis rates. The critical variable was total protein consumed, not meal timing. Jefferson Health's guidance on the topic summarizes it well: "Intermittent fasting can lead to muscle loss, but it doesn't have to," provided you prioritize protein intake and incorporate resistance training.
The people most vulnerable to fasting-related muscle loss are older adults (who already face age-related muscle decline, or sarcopenia), individuals with chronic conditions like diabetes or COPD, and anyone in a severe calorie deficit. For these groups, the Frontiers in Nutrition review explicitly warned that fasting "may have deleterious effects" and recommended against it without medical supervision. Understanding how food quality and research intersect can help contextualize these findings within the broader nutrition evidence landscape.

Who Should Avoid Fasting Entirely
While intermittent fasting is generally safe for healthy adults, several groups should either avoid it entirely or pursue it only under medical supervision. This isn't a matter of preference; it's a matter of genuine health risk.
Pregnant and breastfeeding women should not fast. Caloric restriction during pregnancy is associated with adverse outcomes for both mother and child, and no reputable medical organization recommends fasting during pregnancy or lactation. People with a history of eating disorders, including anorexia, bulimia, or binge eating disorder, should approach fasting with extreme caution. The restriction-and-release cycle of intermittent fasting can trigger or worsen disordered eating patterns, and multiple clinical guidelines flag this as a significant concern.
People taking insulin or sulfonylureas for diabetes face a real risk of hypoglycemia during extended fasting periods. Blood sugar can drop dangerously low when these medications interact with a prolonged absence of food. Any diabetic considering fasting should discuss it with their endocrinologist first and never modify medication schedules without medical guidance.
Children and adolescents should not practice caloric restriction or time-restricted eating for weight loss. Their nutritional needs for growth and development are fundamentally different from adults, and the potential harms of insufficient calorie intake during development outweigh any potential benefit. People recovering from surgery, managing chronic kidney disease, or experiencing malnutrition also fall outside the population for whom fasting has been studied and found safe.
The Metabolic Adaptation Question
A less-discussed but important consideration is metabolic adaptation, sometimes called "starvation mode" in popular media (though that term overstates what actually happens). When you maintain a calorie deficit over weeks or months, your body gradually reduces its energy expenditure. Your resting metabolic rate drops, non-exercise activity (fidgeting, walking, standing) decreases, and the thermic effect of food (energy used to digest meals) declines with fewer eating occasions.
This adaptation happens with any sustained calorie deficit, not just fasting. However, some researchers have hypothesized that the cyclical nature of intermittent fasting, alternating between fasting and feeding periods, might help mitigate metabolic adaptation compared to continuous restriction. The evidence for this hypothesis is mixed at best. A 2023 systematic review in Obesity Reviews found no consistent evidence that intermittent fasting protocols produced less metabolic adaptation than continuous calorie restriction over periods longer than 12 weeks.
What the research does suggest is that protein-sparing mechanisms kick in during fasting as the body shifts to burning ketone bodies derived from fatty acids. This partially protects muscle tissue during shorter fasts, but the protection diminishes with extended fasting periods and severe calorie deficits. The practical implication is straightforward: moderate fasting protocols (like 16:8) with adequate protein intake are unlikely to cause significant metabolic damage, while extreme approaches (multi-day water fasts, very low calorie alternate-day fasting) carry greater risk with limited additional benefit. If you're also looking at ways to reduce exposure to harmful substances in your food, combining that awareness with thoughtful nutrition choices is more sustainable than any crash protocol.
What to Remember
Fasting can help you lose weight, but it does so by reducing calorie intake, not through unique metabolic mechanisms. The latest research from Harvard, the ChronoFast study, and the 2026 Cochrane review all converge on this conclusion. If restricting your eating window makes it easier for you to eat less overall, intermittent fasting is a valid approach. If it leads to compensatory overeating during your feeding window (a common pattern), it won't help.
Protect your muscle mass by maintaining protein intake at or above 1.6 grams per kilogram of body weight daily, distributed across your available meals, and combine any fasting protocol with resistance training. Avoid fasting if you're pregnant, managing diabetes with insulin, recovering from an eating disorder, or under 18. And be skeptical of anyone selling fasting as a metabolic hack that transcends the basic physics of energy balance. The science says it's a useful tool for some people, not a universal solution, and certainly not magic.
Sources
- Intermittent Fasting May Be Effective for Weight Loss, Harvard T.H. Chan School of Public Health
- Scientists Tested Intermittent Fasting Without Eating Less, ScienceDaily
- Intermittent Fasting Offers No Greater Weight Loss Than Standard Diets, Euronews Health
- A Muscle-Centric Perspective on Intermittent Fasting, Frontiers in Nutrition (PMC)
- Intermittent Fasting Can Lead to Muscle Loss, But It Doesn't Have to, Jefferson Health

